🚀 Meet Us at HIMSS 2026 | March 9–12, 2026 | Las Vegas, NV 🎉
.png)
Your MA spends 90 minutes daily doing work an AI should handle in 90 seconds.
Specialty practices run on longitudinal context. Years of encounters, treatment adjustments, and outside records must align before each visit. Pre-charting is a critical clinical work that shapes the patient encounter before it begins.
Today, nursing staff and MAs spend hours assembling histories and tracking external documents across multiple sources and in multiple formats. The process is manual, repetitive, and breaks down at scale.
When pre-charting fails, you walk in cold. You reconstruct timelines while the patient waits. Cognitive load builds across each visit. Clinical risk rises when context is fragmented or missing.
Specialty care needs a different approach: visit readiness for every encounter that protects your team's capacity.
That is what Marvix delivers.
Marvix approaches pre-charting as an active clinical process, preparing the chart before the visit begins. It brings together structured data, clinician inputs, and longitudinal context to ensure the patient record reflects what matters for the upcoming encounter. Here’s how it does it:
Marvix begins pre-charting by pulling clinically relevant information directly from the EHR and connected systems. The focus is on assembling the patient’s clinical history in a way that supports continuity of care and visit readiness.
Marvix brings all of this together before the visit, so clinicians start each consultation with the full clinical picture in view.
Not all clinically relevant information lives inside the EHR. Marvix allows clinicians and care teams to manually upload data that originates outside connected systems, ensuring pre charting reflects the full clinical context, not just what is already structured.
By combining EHR pulled data with manually uploaded inputs, Marvix ensures clinicians walk into every visit with a complete, visit ready view of the patient.
Marvix allows clinicians and care teams to add context before the visit, with a clear focus on prior clinical thinking and accountability.
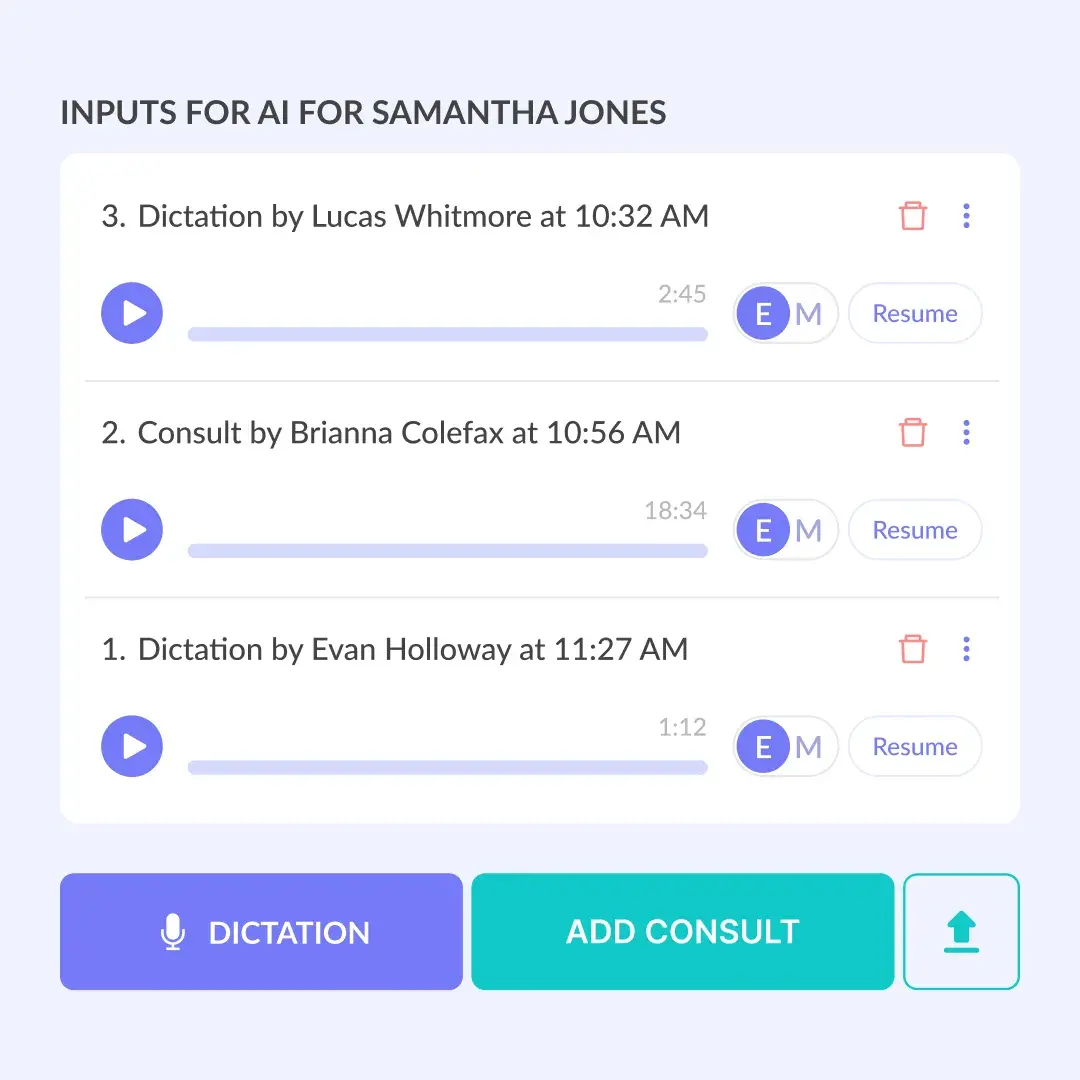
Clinicians can add previous dictations from earlier consults or updates that have not yet been reflected in a formal note. Every entry is automatically displayed with the author’s name and timestamp, so teams can see who added the input and when. All updates made by the team members update in real-time so there’s no delay in information sharing.
This makes multi-user workflows clear and reliable, even when several clinicians or staff members contribute to the same patient visit.
Once all available data is in place, Marvix processes the information through its AI Summarizer and generates a Patient Recap within minutes. This recap brings together EHR data, manually uploaded documents, and prior dictations into a single structured summary that can be reviewed before the consultation begins.
The Patient Recap organizes clinical information by category and time, giving clinicians a clear timeline view of the patient’s history and current context. It includes prior diagnoses, treatments and therapies, unresolved clinical problems, medication histories and changes, and recent labs and imaging. A chronological history connects past encounters to the current visit, while interval summaries highlight what has changed since the last encounter.
The recap can be configured to match the provider’s workflow. Marvix adjusts the level of detail, section order, and terminology style based on specialty and documentation preferences. By ingesting years of notes, labs, and imaging from multiple sources and formats, Marvix produces a longitudinal clinical summary that reduces chart review time and helps clinicians start each visit with complete context.
Let’s take the case of a patient followed in neurology for over five years who is returning for a follow-up visit with a clinician.
The patient is a 67-year-old male with progressive cognitive decline and functional impairment. Over the course of care, he has undergone multiple neurology evaluations, neuropsychological testing, medication trials, and serial brain imaging. Early symptoms included short-term memory loss and word-finding difficulty, which progressed over time to impaired executive function and increasing dependence on caregiver support. His history also includes psychiatry involvement for behavioral symptoms and caregiver-submitted questionnaires documenting functional change.
The patient is now returning after an 18-month gap in neurology care. Since the last visit, medications were adjusted by primary care, new behavioral symptoms were reported by the caregiver, a repeat MRI was completed at an outside imaging center, and functional status declined with emerging safety concerns at home.
The neurologist wants a complete, accurate view of how the patient has evolved before the visit begins. This requires assembling clinical information spread across years, providers, and systems. Let’s look at what all the doctor has to review:
To prepare for this visit, the clinician must understand:
Without Marvix, pre-charting becomes a manual reconstruction process across years of neurology documentation.
Medication histories are reviewed visit by visit, while MRI reports, neuropsychology testing, psychiatry notes, and primary care documentation are opened separately to assess interval change and events during gaps in specialty care.
External inputs, including caregiver questionnaires and outside imaging, must be located across disparate systems and incorporated into context. The clinician then synthesizes these fragmented sources into a coherent longitudinal timeline. Only after that reconstruction can the priorities for the visit be defined.
With Marvix, pre-charting begins before the clinician opens the chart.
Longitudinal neurology documentation, medications, neuropsychology reports, imaging, labs, and primary care notes are aggregated directly from the EHR, with external documents being uploaded in advance. Any dictation inputs ahead of the consult are included with clear attribution and timing.
Once assembled, Marvix generates a structured Patient Recap organized by time and category. Interval changes since the last neurology visit are surfaced within the broader longitudinal context.
The clinician enters the visit with a single, synthesized summary, allowing the encounter to focus on assessment and decision-making rather than reconstruction.

Pre-charting with Marvix changes how clinicians start the visit.
The Patient Recap serves as the clinical foundation for the encounter, carrying forward prior decisions, unresolved problems, and recent changes that matter for the day’s consult. This reduces clinical risk and supports continuity across visits and providers, particularly in complex, longitudinal care. The recap establishes a consistent baseline for every encounter, even in high-volume clinics.
By offloading chart synthesis and longitudinal context building, Marvix lowers cognitive load across the clinical day and allows clinicians to focus on assessment, decision making, and the patient in front of them.
Experience how Marvix’s pre-charting fits into your day before the patient walks in. Start your 30-day free trial of Marvix, customised to your workflow and integrated directly with your EHR.